Coding Compliance Audit Statistics: What to Do With Them?
Coding Compliance Audit Statistics: What to Do With Them?
Why was $100,000 left on the table last quarter? Healthcare organizations and coding consulting companies, often conduct annual coding compliance audits, but do not understand findings generated nor create an action plan. If organizations are unable to turn their data into action plans, they will answer a similar question.
Year by year, organizations rely more and more on their data analytics. In a recent Eaxsol Data Centers survey of 500 businesses worldwide, data is increasingly crucial to the majority of organizations. Eighty percent were unable to function without their data sources. Twenty-five percent totally reliant on statistical metrics in daily operations and decision-making.
In this article you will be provided with:
- An overview of key statistics to include in your coding compliance audits
- A Questionnaire to determine if you need a coding compliance audit program
Compliance Audit Statistics worth Understanding
Each coding compliance audit may have varying scopes depending on annual objectives and budgetary goals. We have identified below the key elements that, in our auditor’s experience, should be audited, reported and most importantly, understood. In order to develop an action plan for each coding compliance audit.
I. Overall Summary Report:
This summary review is meant to provide a high-level overview of the primary indicators. Flagging indicators that deviate from the upper and lower control limits allows you to quickly identify the data sets to examine.
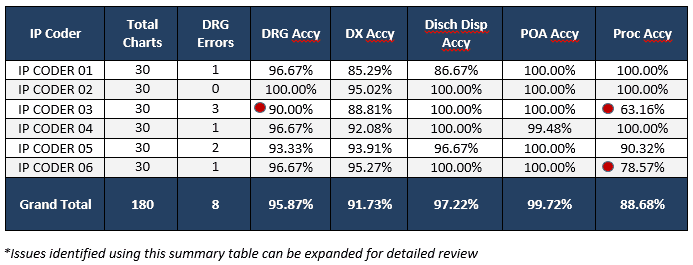
Individual statistical indicators in the summary report:
- MS-DRG or APR-DRG
- Understanding DRG accuracy rates which are directly linked to reimbursement is one of the primary goals for any coding compliance audit.
- Identify which coders need additional education, focused audits, or pre-bill secondary reviews.
- Discharge Disposition
- In some cases, the discharge dispositions may drive DRG changes.
- A detailed review will allow you to identify if the coder doesn’t understand what types of facilities the patients are being transferred to or if the issue is as simple as the coder may be working from outdated facility listing.
- Present on Admission (POA)
- Understanding the POA accuracy rate is important because this indicator is tied to multiple quality initiatives.
- If POA is not identified properly it will affect both quality and complications statistics.
- This could negatively affect facility report cards leading to decrease reimbursements or potential fines.
- Diagnosis (ICD-10-CM) Code Assignments
- Understanding your diagnosis accuracy breakdown allows you to isolate what diagnosis issues are driving your DRG changes.
- Detailed review will provide insight into Principal Diagnosis (PDX) vs. Secondary Diagnosis (SDX).
- Inaccurate PDX assignments often drive DRG changes while SDX statistics allow you to identify if any CC/MCC issues are present which also drive DRG changes.
- Procedure (ICD-10-PCS) Code Assignments
- Understanding ICD-10-PCS assignments allows you to categorize errors to establish the root cause impacting the DRG.
- As mention in example #2, the ICD-10-PCS accuracy statistics examine if the issue was with the approach, root operation, body system, device or body part.
A “deeper dive”:
Example #1 (IP Coder 03)
- Indicator #1 flagged – 90% DRG accuracy rate: A detailed review includes reviewing the DRG Classifications to assess if it requires targeted education or a focused audit.
- Important questions to ask in this scenario: Is the coder inaccurately assigning code(s) around same concept, a specific facility guideline, or AHA Coding Clinic? Would the coder benefit from a coding refresher course(s)? Or do they need a focused audit?
 Another option in this case could be to place coder into a pre-bill secondary review coder mentoring program (more information here on a recent case study we published on the positive impact of Coder Mentoring programs on coding accuracy.)
Another option in this case could be to place coder into a pre-bill secondary review coder mentoring program (more information here on a recent case study we published on the positive impact of Coder Mentoring programs on coding accuracy.)
- Indicator #2 flagged – Secondary to the DRG Accuracy, we flag educational opportunities for procedure (ICD-10-PCS) code assignment. In this case, when diving “deeper” into our audit findings reports, ICD-10-PCS procedure code inaccuracies cause the majority of the DRG changes. Additional ICD-10-PCS education was provided and, in the next audit, both DRG as well as ICD-10-PCS accuracy rates improved.
Example #2 (IP Coder 06)
- Indicator #1 flagged – 78.5% ICD-10-PCS accuracy rate.
- The coder exceeded the national industry standard of 95% DRG accuracy, however clearly identified education opportunities exist related to ICD-10-PCS code assignments (78.5%).
- Detailed understanding of the ICD-10-PCS accuracy statistics can identify the specificity of the errors (by approach, root operation, body system, device or body part.)
II. Financial Impact Report based on DRG Changes:
The financial impact analysis report outlines overcoded cases and undercoded cases along with MDC groupings. Strategically, you re-bill any undercoded cases in order to capture accurate documentation-proven additional reimbursement originally “left on the table.” Conversely, by law, you need to re-bill all Medicare overcoded cases in accordance with the Medicare rules/regulations.

While reviewing the financial impact report, it is imperative healthcare organizations and coding companies understand the following data points from the compliance audit statistics:
- Number (#) of DRG Changes per MDC Grouping
- Outlines where focused educational opportunities are present and/or focused audits need to be conducted.
- Example – In the 1Q19 Financial Impact Report listed on page 3, we recommend a refresher course for your entire coding team on “Gastrointestinal Diagnoses” or “Gastrointestinal Procedures.” (Over half 48/87 DRG changes occurred in that DRG grouping.)
- Overall breakdown of overcoded vs. undercoded cases
- Specific education topic recommendations
- A secondary benefit to each audit is the ability to highlight the current strengths and weakness of your coding staff.
- At YES HIM Consulting, Inc., we believe education is the foundation for success and thus include specific educational course recommendations with each audit.
III. Accuracy Stats by Coder Report

- Leverage the statistics by coder to identify specific coder issues vs. entire coding team issues
- Examining each coder’s accuracy rate may indicate a lack of knowledge on a specific AHA Coding Clinic. Or, it may identify that all coders had issue with same facility policy that maybe wasn’t communicated adequately.
IV. Accuracy Stats by Facility Report

- Leverage the statistics by facility to identify specific facility issues
- A detailed understanding of the facility delineation will highlight if multiple facilities are having the same issue or if each facility has unique educational opportunities.
- Examine any coder / facility accuracy trends as well as MDC/DRG trends for additional education and/or focused audits.
V. Detailed Documentation of Coder Review Sheets
- Coders and their supervisor use Coder Review Sheets to vet (i.e. agree or disagree) with the draft audit findings.
- We believe so strongly that education is the foundation of the audits. So, we use the vetting process as an opportunity to foster communication with the coders. The process keeps them engaged and informed.
- VALUE ADDED – Coding staff let down their barriers and realize our auditing team is there to help them. And not look over their shoulders and judge them!
Your facility could be at risk if you operate under the pretense that your coding compliance audit program is only for a once-a-year compliance checkbox. If management doesn’t take the time to delineate, evaluate and understand the statistical data. They pose the risk of making uninformed decisions that could result in unattended consequences downstream (Journal of AHIMA, 2009).
Do I Really Need an External Compliance Audit Completed? – Questionnaire
Interested in obtaining the value created from a coding compliance audit but not sure if you want to complete it internally or externally? Complete our Compliance Audit Questionnaire below:
Compliance Audit questionnaire by YES
Whether your approach is conducting your coding compliance audits internally or externally, or a mix of both, if you take the time to understand what the data indicators are telling you…your organization will see quality improvements in your coding capabilities. For additional expertise on the benefits of coding compliance audits, review these articles: “External Coding Audits: How They Directly Affect the Success of Your Organization,” and “Compliance Audits Shed Light on Performance Improvement in Medical Coding.”


