The Importance of Project Management in Healthcare & Its Role in HIM
The Importance of Project Management in Healthcare & Its Role in HIM
Today’s healthcare leaders continuously refine and develop their processes to improve patient care, reduce costs and elevate the patient’s overall experience and satisfaction. Adopting of project management (PM) principles in healthcare has dramatically increased over the last decade. It has become increasingly important to facilities because they help control costs, mitigate risk, and improve overall project outcomes. There are a vast number of electronic system implementations (i.e., EHRs, CACs, CDI Software, etc.) within healthcare. As a result, project management has emerged as one of the most prominent business skill sets desired. YES’ Consultants are specifically trained as project managers and can help your organization develop a plan to successfully achieve your goals. Contact YES for more information on how project management can benefit your facility!
One area within healthcare where we have seen project management significantly add value to organizations is Health Information Management (HIM). Historically, if you were to ask any HIM professional if they need assistance initiating, planning, executing, monitoring, and closing projects or processes, the majority would unequivocally tell you that they or their supervisors had adequate time to complete all their tasks/projects.
Unfortunately, in our experience, we have found that not to be the case. Oftentimes, Vice Presidents or C-suite executives assign additional high-priority, time-consuming projects to their HIM leadership teams. With hospitals cutting costs in recent years, HIM teams have been asked to do even more with fewer resources. Many HIM departments are constantly under pressure to manage concurrent priorities against the facility’s DNFB. As a result, time constraints arise for many other activities, especially retrospective projects.
Project management principles will allow HIM departments to generate value from their various retrospective activities if utilized properly. This includes audits while maintaining focus on their concurrent priorities.
In this article, we will outline:
- Common Challenges HIM Leaders Encounter
- Project Management (PM) Strategies and Approach for HIM
Common Challenges HIM Leaders Encounter
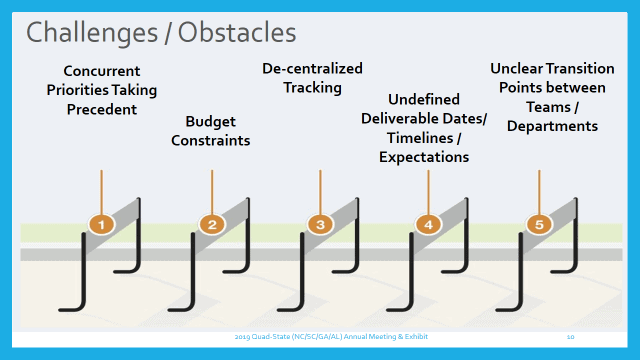
Concurrent Priorities Taking Precedent – Day-to-day operations within HIM departments fluctuate frequently. As an HIM leader, it may seem like your full-time job is putting out fires related to your duties (i.e., managing your DNFB). In this environment, your daily state of mind is set to “crisis management mode.” By employing the basic project management principles outlined, you can balance staffing needs, physician needs, patient volume fluctuations, supervisor or C-suite delegating tasks, and other priorities properly.
Budget Constraints – Financial performance against your budgets can be very demanding. Oftentimes, budgeting constraints impede HIM leaders from implementing important retrospective audit activities.
More Challenges That Plague HIM Leaders
Decentralized Tracking – With HIM departments managing many different projects or teams (i.e., Coding, Auditing, Transcription, CDI, etc.) on a daily basis, accurate and timely tracking of current activities presents a challenge. Add in the fact that many HIM teams, such as coding and transcription, are employing increasingly more remote staff, and you could have a recipe for failure if not properly project-managed.
Undefined Timelines and Expectations – The development of timelines and clearly identified expectations can be easily bypassed as more “higher priority” tasks take precendence. A significant challenge many HIM leaders face is having the actual daily time to develop and communicate clear deadlines or expectations.
Unclear Transition Point between Teams or Team Members – Very rarely do HIM projects or processes involve a single individual or single team. The largest risk for miscommunication arises when transition points (“handoffs”) between teams or team members lack clear identification.
Project Management (PM) in Healthcare Examples and Approach that Add Value to Your Organization
As healthcare in the United States continues to evolve under mounting cost and quality pressures, the need for project management becomes ever more apparent. Understanding and applying the foundations of project management can significantly improve outcomes across healthcare delivery settings.
Below are five Project Management Best Practices you can apply to any HIM project/process today to generate more efficiencies.
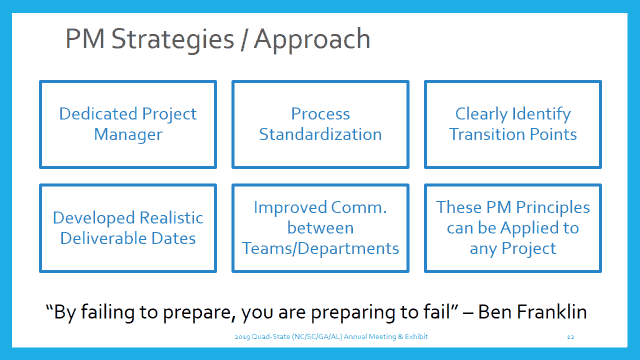
Project Management Best Practices
In today’s dynamic ever-changing healthcare environment, centralized tracking efforts are what we need to strive for. In response, a dedicated HIM project manager sets the foundation for success. The PM tracks, communicates, and facilitates all transition points between teams and departments.
NOTE: If your team or department doesn’t have access to a dedicated Project Manager…any dedicated resource within the organization with good communication skills will be helpful.
The second project management best practice to employ across all initiatives is process standardization. There are three main benefits of standardizing your processes:
- Higher Productivity & Output – By having more efficient processes, you’ll end up with higher productivity across the organization.
- Easier Process Improvement – Process standardization will lay the foundation for more agile process improvement initiatives in the future.
- Easier Onboarding – If you have a standardized process, it’s easier for new employees to be brought up to speed. Otherwise, working on different teams would require them to re-learn some of the process steps.
Next, you need to clearly identify each transition point between teams and/or departments. This particular project management best practice significantly decreases your risk of communication breakdowns.
Our fourth project management best practice is the development of realistic deliverable dates. When developing your target dates, account for lead/lag time (essentially “buffer” time) around your competing priorities. Selecting those realistic target dates will allow you to find the balance between working on your concurrent priorities while still realizing value from your retrospective activities.
The fifth project management best practice is fostering and improving communication between the different teams/departments. In our experience, it is vital that you institute a multi-disciplinary approach at the onset of any project.
Conclusion
Adopting certain project management strategies equips you with the tools to thrive in the chaotic environments in which we operate. I would offer that “PM” does not need to stand for project management. But, rather, let it stand for Peace of Mind. Peace of mind knowing that with these strategies, your projects and processes will be more efficient. They will generate more value for not only you but your entire organization. YES’ Consultants are specifically trained as HIM project managers and can help your organization develop a plan to successfully achieve your goals. Contact YES for more information on the importance of project management in healthcare and how it can benefit your facility!


